🕐 Read Time: 6 min
RCM Medical Billing in Texas: Stop Revenue Loss Before Denials Happen
Walk into any medical practice in Texas on a Tuesday afternoon, and you will see the same pattern playing out.
Someone at the front desk is on hold with an insurance company, trying to verify coverage that should have been confirmed last week. A provider is running 20 minutes behind because the previous appointment took longer than scheduled. The billing coordinator is finishing chart notes from yesterday while juggling coding for today’s visits. By 6 PM, claims go out with a small but costly mistake buried in the details.
Three weeks later, the denial letter arrives. Now the entire team starts over, resubmitting paperwork and chasing payments that should have arrived weeks ago.
This cycle repeats itself thousands of times across Houston, Dallas, Austin, San Antonio, and beyond. The problem is not that anyone is doing their job poorly. The problem is that traditional RCM medical billing systems create friction at every step.
Why Traditional RCM Medical Billing Systems Create Revenue Leaks
When we talk to practice managers across Texas, they describe the same challenge: their RCM medical billing workflow lives in too many disconnected places.
Scheduling happens in one system. Patient demographics get entered separately. Insurance verification requires phone calls or separate portals. Clinical notes live in the EHR. Billing software pulls data through exports. Someone manually reconciles everything, hoping nothing falls through the cracks.
But things do fall through. A coverage change that should have been caught at registration. A documentation detail that makes a code inappropriate. An authorization requirement that nobody flagged. These are not dramatic failures. They are quiet, expensive mistakes that compound over time.
Edvak takes a different approach to RCM medical billing. Instead of adding another disconnected tool to your workflow, we built a platform where eligibility checks, documentation, coding assistance, claims validation, and patient payments work as one connected system.
Four Ways Edvak's RCM Medical Billing Platform Protects Revenue Before Problems Start
Insurance Verification That Actually Prevents Surprises
Most practices verify insurance, but they do it too late or without enough detail to catch problems.
Edvak’s Real-Time Insurance Checks run the moment an appointment is scheduled. The system pulls comprehensive benefit details including active coverage status, deductible progress, copay amounts, coverage limits, and authorization requirements. When something looks wrong, maybe expired coverage or a plan change, your front desk sees it immediately with enough time to resolve the issue before the patient arrives.
For Texas practices managing patients with employer plans, Medicaid, Medicare, and marketplace coverage, this early visibility prevents the most common source of denials. You are not scrambling at check-in. You are not discovering coverage issues three weeks after the visit when the claim gets rejected.
What this means for your practice:
- Coverage verified automatically, not through phone calls
- Authorization requirements identified before the appointment
- Accurate cost estimates ready when patients ask
- Fewer “patient not eligible” denials that waste team time
AI That Suggests Codes Instead of Making Your Staff Hunt for Them
Coding errors are not usually about incompetence. They happen because coders and billers are moving fast, working from incomplete notes, and keeping hundreds of payer rules in their heads.
Edvak’s AI-Assisted Medical Coding reads clinical documentation as it is completed and suggests ICD-10 diagnosis codes and CPT procedure codes that match what the provider documented. The system validates these suggestions against current billing rules and payer-specific requirements before anyone clicks submit. Your coding team reviews the context and approves accurate codes in seconds instead of searching through manuals.
This is particularly valuable for Texas practices billing to Blue Cross Blue Shield of Texas, UnitedHealthcare, Aetna, and dozens of smaller regional plans, each with their own coding preferences and bundling rules.
What this means for your practice:
- Codes suggested based on actual documentation, not guesswork
- Validation happens before submission, not after denial
- Consistency across multiple coders and providers
- Less time spent on rework from coding mistakes
Claims Validation That Catches Mistakes Your Team Would Never See
The claims that get denied are rarely obviously wrong. They have subtle mismatches that slip past manual review but trigger automatic rejections from payer systems.
Edvak’s Claims Management includes pre-submission scrubbing that checks every claim against hundreds of validation rules. Patient demographics match insurance records exactly. Procedure codes align with diagnosis codes. Service dates fall within coverage periods. Authorization numbers are present when required. The claim format meets the specific requirements of each payer.
When something fails validation, the system explains exactly what is wrong so your team can fix it before the claim leaves your practice. Once submitted, real-time tracking shows you exactly where each claim stands without having to log into multiple payer portals.
What this means for your practice:
- Higher first-pass acceptance rates
- Fewer claims stuck in processing limbo
- Faster identification of actual problems
- Less time spent manually following up
Patient Payment Tools That Feel Like 2025, Not 2005
Patient responsibility keeps growing across Texas as high-deductible plans become standard. Yet many practices still send paper statements and wait for checks in the mail.
Edvak’s Patient Payment platform gives patients clear digital statements, multiple payment methods including cards and digital wallets, and the ability to set up payment plans themselves without calling your office. Automated reminders keep balances visible without your team making awkward collection calls.
For larger balances that patients cannot pay immediately, the system supports recurring payment arrangements that patients configure through the portal. This keeps them current while improving your collection rates without adding pressure to your staff.
What this means for your practice:
- Payments arrive faster because the process is convenient
- Less staff time spent on collections
- Better patient satisfaction with transparent billing
- Healthier accounts receivable aging
What Integration Actually Looks Like in Daily Practice
Here is how a typical patient visit flows when everything is connected:
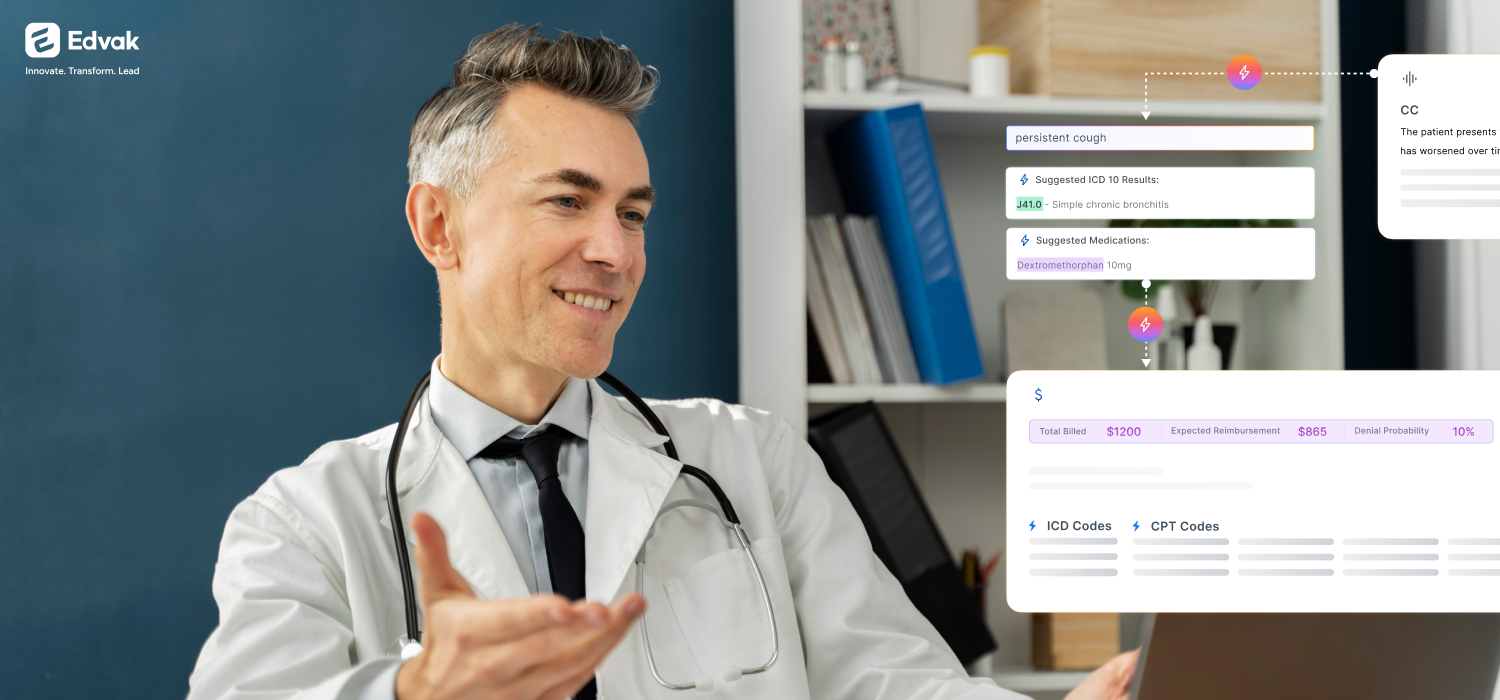
The patient schedules online or through your front desk. Eligibility verification runs automatically, pulling current benefit details and flagging any issues. Your team sees that the patient’s deductible is nearly met and pre-authorization is required for the planned procedure. They obtain the authorization before the appointment day.
The patient arrives. Check-in is smooth because coverage and financial responsibility were confirmed in advance. The provider sees the patient and completes documentation using Darwin AI, Edvak’s ambient documentation tool that captures structured clinical notes.
After the visit, AI-assisted coding reviews the documentation and suggests appropriate codes with full context visible. Your billing coordinator reviews and approves in seconds. Pre-submission validation confirms the claim is clean. It routes to the correct payer with all required information.
The claim processes without issues. Payment posts automatically. The patient receives a clear statement showing what insurance paid and what they owe. They pay online in two clicks.
Nothing heroic happened. That is the entire point. The system prevented problems instead of forcing your team to fix them later.
Built for How Texas Practices Actually Operate
Edvak works for solo practitioners in small Texas towns and multi-provider groups in major metro areas. It handles primary care practices seeing 50 patients daily and specialty clinics with complex coding requirements.
The platform integrates with the EHR systems commonly used across Texas through standard protocols like HL7 and FHIR. This means no duplicate data entry and no exporting files between systems. Clinical documentation flows directly into billing workflows without manual transfers.
When you combine Edvak’s billing platform with Darwin AI for clinical documentation, you create an end-to-end workflow where every piece of information flows smoothly from the patient encounter through final payment. Better documentation leads to more accurate coding. Accurate coding leads to cleaner claims. Cleaner claims get paid faster.
The Real Cost of Doing Nothing
Every denied claim costs your practice money in three ways.
First, you lose the time your team spends on rework. Someone has to identify the problem, gather missing information, correct the claim, and resubmit. That same person could have been working on new claims or other revenue-generating activities.
Second, you lose the time value of money. A claim that should have paid in 20 days now takes 60 or 90 days to resolve. That delayed cash flow affects everything from payroll to purchasing decisions.
Third, you lose revenue permanently. Industry research shows that 50-65% of denied claims never get resubmitted. Your team gets busy with new claims and denials pile up until they are written off.
For a typical Texas practice, these losses add up to thousands of dollars monthly. Over a year, that is enough to hire another staff member, upgrade equipment, or simply improve profitability.
Is This Right for Your Texas Practice?
Edvak makes sense for practices that are:
Tired of preventable denials. If your team spends significant time fixing claims that should have been right the first time, automated validation and AI-assisted coding eliminate most of those problems.
Struggling with cash flow. When claims sit for 60-90 days instead of 20-30 days, your working capital suffers. Cleaner claims and faster processing improve cash flow noticeably.
Dealing with staffing constraints. Texas practices face the same hiring challenges as everywhere else. When your team is lean, efficiency tools like Edvak let them accomplish more without working longer hours.
Growing and needing consistency. As practices add providers and locations, maintaining billing consistency becomes harder. Integrated workflows and AI assistance ensure everyone follows the same standards.
Working with complex payer mixes. Texas practices often bill to Medicare, Medicaid, major commercial insurers, and regional plans. Managing all those different requirements manually is exhausting. Automated validation handles the complexity.
Common Questions Texas Practices Ask About RCM Medical Billing
-
What is RCM medical billing?
RCM medical billing stands for Revenue Cycle Management medical billing, covering the complete financial process from patient registration through final payment collection. This includes insurance verification, medical coding, claim submission, payment posting, and denial management. Edvak's RCM medical billing platform manages this entire cycle for Texas practices in one integrated system, ensuring nothing falls through the cracks between steps.
-
What are the key steps in RCM medical billing?
RCM medical billing includes patient registration and insurance verification, charge capture and documentation, medical coding with ICD-10 and CPT codes, claims submission and validation, payment posting and reconciliation, denial management and appeals, and patient balance collection. Edvak automates and connects each step so Texas practices catch errors early and reduce rework throughout the entire RCM medical billing process.
-
Why is RCM medical billing important for Texas practices?
Effective RCM medical billing ensures Texas practices get paid accurately and quickly for services provided. Without proper RCM medical billing processes, practices face delayed payments, high denial rates, cash flow problems, and lost revenue from claims that never get resubmitted. Edvak's RCM medical billing platform prevents these issues by validating claims before submission and tracking payments throughout the entire cycle.
-
How quickly can Texas practices see results from better revenue cycle management?
Most practices notice cleaner claims within the first week and fewer denials within 30 days. Cash flow improvements typically appear within 60-90 days as cleaner claims process faster and fewer get stuck in denial cycles. Edvak's real-time eligibility verification starts protecting revenue immediately by catching coverage issues before services are provided.
-
What should Texas practices look for in RCM software?
The most important factors are integration with your existing EHR, automation that reduces manual work, real-time validation before claims are submitted, clear visibility into claim status, and patient payment tools that match consumer expectations. Edvak checks all these boxes and adds AI-powered coding assistance that most standalone billing systems lack.
-
How does Edvak handle different insurance plans common in Texas?
What happens if a claim still gets denied even with validation? Edvak validates claims against payer-specific requirements for Medicare, Medicaid, Blue Cross Blue Shield of Texas, UnitedHealthcare, Aetna, Humana, and hundreds of other plans. The system knows the formatting rules, authorization requirements, and coding preferences for each payer. Texas practices benefit from this built-in intelligence without maintaining complex internal payer rule databases.
-
What happens to patient responsibility as deductibles keep rising in Texas?
Patient balances now represent 30% or more of revenue for many Texas practices. Traditional collection methods like paper statements and phone calls no longer work well. Edvak's Patient Payment platform gives patients the digital payment experience they expect, with clear statements, multiple payment options, automated reminders, and self-service payment plans that improve collection rates without burdening staff.
-
Does implementing new RCM software disrupt practice operations?
Edvak integrates with existing EHR systems through standard protocols, so clinical workflows continue unchanged. The billing team transitions gradually, starting with eligibility checks and claims validation while maintaining their current processes. Full implementation typically completes within 30-60 days with minimal disruption to daily operations in Texas practices of any size.
-
How much revenue do Texas practices lose to preventable denials annually?
With denial rates between 5-15% and over half of denials never resubmitted, a Texas practice collecting $1 million annually could lose $50,000-$100,000 to preventable denials and abandoned claims. Factor in staff time spent on rework, and the real cost is often higher. Edvak helps practices recover this lost revenue by preventing denials before they happen.
-
Can smaller Texas practices benefit from advanced RCM tools?
Absolutely. Smaller practices often feel denial impacts more severely because they have fewer resources to dedicate to rework. Edvak scales to practices of any size, from solo providers to large groups. The automation and AI assistance are actually more valuable when staff is limited, letting small teams perform at the level of much larger billing departments.
-
What is the typical return on investment for RCM software in Texas?
Most Texas practices see ROI within 3-6 months through reduced denials, faster payments, improved collection rates, and staff time savings. A practice that prevents just 2-3% of its claim volume from denial while collecting patient balances 20% faster typically recovers the software investment quickly. Edvak's transparent pricing makes the ROI calculation straightforward.
-
How does Edvak keep up with constantly changing billing regulations?
The platform updates automatically as coding guidelines change, payer rules evolve, and compliance requirements shift. Texas practices do not need to manually update validation rules or retrain AI models. These updates happen behind the scenes, ensuring your claims always meet current standards without additional work from your team.
-
What kind of support do Texas practices receive during implementation?
Edvak provides dedicated implementation support, training for your team, integration assistance with your EHR, and ongoing customer success resources. We understand that Texas practices range from small clinics to large multi-location groups, so support is customized to your specific situation, patient volume, and specialty requirements.
-
Can practices track specific metrics that matter for revenue cycle performance?
Edvak provides clear dashboards showing denial rates, days in accounts receivable, collection percentages, claim processing times, and other key performance indicators. Texas practice managers can identify trends, spot problems early, and demonstrate improvement to stakeholders. Real-time data replaces the month-end reports that most practices struggle to generate manually.
-
How does real-time eligibility verification work for Texas Medicaid and CHIP?
Edvak connects directly to eligibility systems for Texas Medicaid, CHIP, Medicare, and commercial payers. The verification happens automatically when appointments are scheduled, pulling current coverage status, benefit details, and authorization requirements. This is especially valuable for Texas practices serving diverse populations with frequently changing Medicaid coverage.
-
What makes Edvak different from traditional medical billing services?
Traditional billing services handle claims submission but typically do not address upstream issues like eligibility verification, coding assistance, or patient payment collection. Edvak gives Texas practices complete control of their revenue cycle with tools that prevent problems rather than just processing claims. You maintain ownership of the entire workflow while gaining automation that improves results.
-
How secure is patient data in cloud-based RCM platforms?
Edvak is fully HIPAA compliant with encryption for data in transit and at rest, regular security audits, access controls, and comprehensive business associate agreements. Texas practices can confidently use the platform knowing patient information is protected according to federal healthcare data security standards and industry best practices.
-
Can Edvak help with Texas-specific reporting requirements?
Yes. The platform generates reports needed for Texas Medical Board requirements, quality programs, and payer audits. Custom reporting allows Texas practices to extract the specific data they need for credentialing, accreditation, or internal analysis without manually compiling information from multiple systems.
-
What happens if a claim still gets denied even with validation?
Denials will occasionally happen even with thorough validation, usually due to post-service issues like coordination of benefits or medical necessity reviews. When denials occur, Edvak provides clear context about why the claim was rejected and what information is needed to resolve it. This speeds up the resolution process significantly compared to deciphering cryptic denial codes manually.
-
How do Texas practices typically price their RCM software investment?
Pricing models vary but typically include per-provider fees, per-claim fees, or percentage-of-collections arrangements. Edvak offers transparent pricing that scales with practice size and needs. Most Texas practices find the investment pays for itself through denial reduction and faster payments within the first few months of use.
See How This Works for Your Practice
Every Texas practice has unique challenges based on specialty, patient demographics, payer mix, and size. The best way to understand how Edvak would improve your specific revenue cycle is to see it in action.
Try Edvak and experience the difference that connected workflows make for billing efficiency and revenue protection.
Want a guided walkthrough tailored to your Texas practice? Schedule a demo with our team.
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



