🕐 Read Time: 6 min
RCM Medical Billing in California: Eliminate Revenue Leakage with Prevention-First Technology
Visit any physician’s office in California during peak hours and you’ll witness a familiar scene unfolding.
The receptionist is waiting on hold with a payer, attempting to confirm patient eligibility that should have been verified days earlier. A clinician is falling behind schedule because the last consultation required extra documentation time. Meanwhile, the billing specialist is catching up on clinical notes from previous days while managing today’s coding workload. When the day ends and claims finally get submitted, a minor oversight buried somewhere in the data goes unnoticed.
Four weeks later, the rejection notice shows up. The entire process must restart: gathering documentation, correcting information, and resubmitting claims that should have been paid a month ago.
This scenario plays out daily in medical offices from San Diego to Sacramento, from the Bay Area to the Central Valley. The issue isn’t staff competence or effort. The fundamental problem is that conventional RCM medical billing approaches introduce obstacles at every stage of the revenue cycle.
Why Conventional RCM Medical Billing Methods Drain Practice Revenue
Practice administrators throughout California in cities like Los Angeles and San Francisco consistently describe identical frustrations: their RCM medical billing operations exist across fragmented, disconnected platforms.
Appointments get scheduled in one application. Demographics are captured separately. Eligibility verification demands phone calls or accessing different portals. Clinical AI documentation resides in the EHR. Billing applications import data through file transfers. Staff members manually cross-reference everything, hoping critical details don’t get missed.
Yet details do get missed. An insurance change that should have been identified during registration. A documentation element that invalidates a particular code. A prior authorization need that nobody caught. These aren’t catastrophic errors they’re subtle, costly oversights that accumulate steadily.
Edvak delivers a fundamentally different RCM medical billing solution. Rather than introducing yet another isolated tool into your operations, we’ve developed an integrated platform where eligibility verification, documentation support, coding intelligence, claims checking, and patient collections function as a unified ecosystem.
Four Critical Ways Edvak's RCM Medical Billing Platform Safeguards Revenue Proactively
Real-Time Eligibility Verification That Eliminates Patient Coverage Surprises
Many practices perform insurance verification, but they execute it too late or without sufficient depth to identify potential issues.
Edvak’s Instant Eligibility Verification activates immediately when appointments are booked. The platform retrieves detailed benefit information including current coverage validity, deductible status, copayment amounts, plan limitations, and prior authorization needs. When irregularities appear perhaps lapsed coverage or plan modifications your front office receives immediate alerts with adequate time to address concerns before patients arrive.
For California practices in Sacramento and Long Beach serving patients with diverse insurance types including employer-sponsored plans, Medi-Cal, Medicare Advantage, and Covered California marketplace options, this advance visibility prevents the leading cause of claim rejections. Your team isn’t firefighting during check-in. You’re not learning about coverage problems a month later when rejections arrive.
Benefits for your practice:
- Coverage confirmed automatically without phone queues
- Authorization needs flagged ahead of scheduled visits
- Precise cost estimates available when patients inquire
- Reduced “eligibility not found” denials that consume valuable staff hours
Intelligent AI That Recommends Codes Rather Than Forcing Manual Searches
Coding mistakes rarely stem from lack of knowledge. They occur because coding staff work under time pressure, interpret incomplete documentation, and attempt to remember countless payer-specific guidelines.
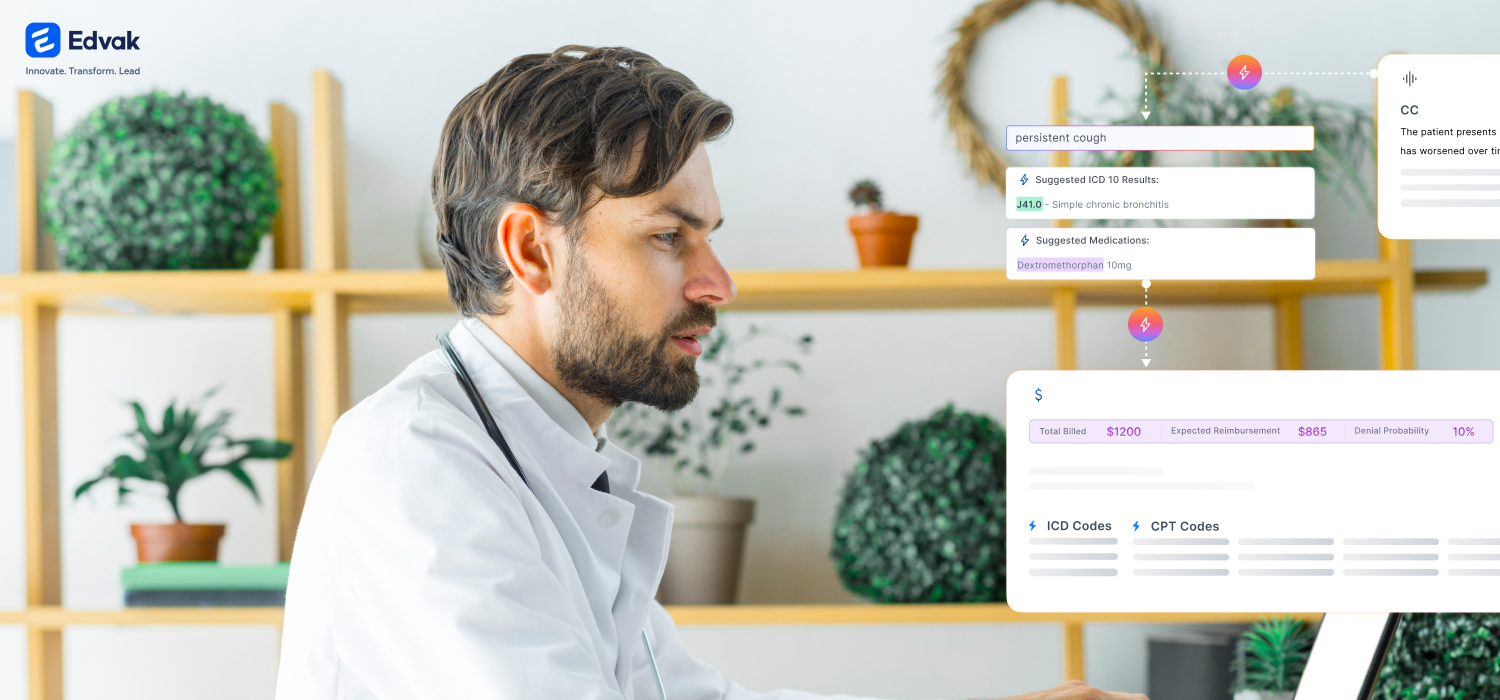
Edvak’s Intelligent Medical Coding analyzes clinical documentation in real-time and recommends appropriate ICD-10 diagnosis codes and CPT procedure codes aligned with provider notes. The platform cross-checks these recommendations against current billing standards and insurer-specific policies before submission. Your coding specialists review contextual suggestions and approve accurate codes within moments rather than searching reference materials.
This capability proves especially beneficial for California practices submitting claims to Blue Shield of California, Anthem Blue Cross, Kaiser Permanente, Health Net, and numerous smaller regional carriers each maintaining distinct coding conventions and bundling regulations.
Benefits for your practice:
- Codes generated from documented clinical findings, not estimation
- Validation completed before submission rather than after rejection
- Uniformity maintained across multiple coding staff and providers
- Significantly reduced time addressing coding-related rework
Pre-Submission Claims Validation That Identifies Errors Invisible to Manual Review
Claims that face rejection are seldom obviously incorrect. They contain nuanced discrepancies that bypass human review but trigger automated payer system rejections.
Edvak’s Claims Processing System incorporates comprehensive pre-submission analysis that examines every claim against extensive validation criteria. Patient information perfectly matches insurance records. Procedure codes properly correlate with diagnosis codes. Service dates occur within active coverage windows. Authorization references appear when mandated. Claim formatting adheres to individual payer specifications.
When validation identifies problems, the platform provides explicit explanations enabling your team to resolve issues before claims leave your organization. After submission, continuous tracking displays precise claim status without requiring logins to multiple payer websites.
Benefits for your practice:
- Substantially improved initial acceptance percentages
- Fewer claims delayed in processing queues
- Quicker identification of genuine issues requiring attention
- Reduced manual follow-up workload
Modern Patient Payment Solutions That Match Contemporary Consumer Expectations
Patient financial responsibility continues expanding across California in cities like San Diego and Anaheim as high-deductible health plans become the norm. Despite this shift, numerous practices still mail paper bills and await mailed payments.
Edvak’s Patient Payment Solution delivers transparent digital statements, diverse payment options including credit cards and digital wallets, and patient-initiated payment plan capabilities without office calls. Automated notifications maintain balance visibility without staff making uncomfortable collection calls.
For substantial balances patients cannot immediately satisfy, the platform enables recurring payment schedules that patients configure independently through the portal. This maintains account currency while enhancing collection rates without adding staff pressure.
Benefits for your practice:
- Accelerated payment receipt through convenient processes
- Decreased staff time dedicated to collections activities
- Enhanced patient satisfaction through transparent billing
- Improved accounts receivable aging metrics
What True Integration Delivers in Daily Operations
Here’s the patient journey when systems work cohesively:
A patient schedules through your online portal or with reception. Eligibility verification executes automatically, retrieving current benefit details and identifying any concerns. Your team discovers the patient’s deductible is almost satisfied but the planned service requires prior authorization. They secure authorization before the appointment date.
The patient arrives for their visit. Check-in proceeds smoothly because coverage and financial obligations were confirmed beforehand. The provider completes the encounter and documents using Darwin AI, Edvak’s ambient documentation solution that generates structured clinical records.
Following the visit, AI-powered coding analyzes the documentation and suggests appropriate codes with complete context displayed. Your billing coordinator reviews and confirms within seconds. Pre-submission validation verifies claim accuracy. It routes to the appropriate payer with complete required information.
The claim processes successfully. Payment posts automatically. The patient receives an understandable statement showing insurance payment and remaining balance. They complete payment online immediately.
Nothing extraordinary occurred. That’s precisely the objective. The system prevented problems rather than forcing your team into reactive mode.
Designed for California Practice Realities
Edvak serves solo practitioners in rural California communities like Stockton and multi-physician organizations in metropolitan centers like Los Angeles and San Francisco. It accommodates primary care offices seeing dozens of patients daily and specialty practices with sophisticated coding requirements.
The platform connects with EHR systems prevalent throughout California using standard protocols including HL7 and FHIR. This eliminates redundant data entry and file transfers between systems. Clinical documentation flows seamlessly into billing workflows without manual intervention.
When combining Edvak’s billing platform with Darwin AI for clinical AI documentation, you establish comprehensive workflow continuity from patient encounter through final payment receipt. Superior documentation produces more precise coding. Precise coding generates cleaner claims. Cleaner claims receive faster payment.
The Hidden Cost of Maintaining the Status Quo
Each rejected claim costs your practice through three distinct channels.
First, you sacrifice staff time on corrections. Someone must diagnose the issue, compile missing information, amend the claim, and resubmit. That individual could have processed new claims or other revenue-generating tasks.
Second, you lose money’s time value. A claim that should have paid within three weeks now requires two or three months to resolve. That delayed cash flow impacts everything from staff compensation to equipment acquisition.
Third, you permanently lose revenue. Industry data reveals that 50-65% of rejected claims never receive resubmission. Your team becomes occupied with current claims while rejections accumulate until they’re written off.
For typical California practices in Santa Rosa and San Jose, these losses reach thousands monthly. Annually, that represents enough capital to add staff, upgrade technology, or simply enhance profitability.
Is This Solution Right for Your California Practice?
Edvak delivers value for practices that are:
- Frustrated with preventable rejections. If your team invests substantial time correcting claims that should have been accurate initially, automated validation and intelligent coding eliminate most problems.
- Experiencing cash flow challenges. When claims remain outstanding for 60-90 days instead of 20-30 days, your working capital suffers. Cleaner claims and expedited processing produce noticeable cash flow improvements.
- Facing staffing limitations. California practices confront the same recruitment challenges as other markets. When your team operates lean, efficiency tools like Edvak enable greater productivity without extended hours.
- Expanding and requiring standardization. As practices add clinicians and sites, maintaining billing consistency becomes increasingly difficult. Integrated workflows and AI assistance ensure standardized processes organization-wide.
- Managing diverse payer portfolios. California practices frequently bill Medicare, Medi-Cal, major commercial insurers, and regional plans. Managing these varied requirements manually proves exhausting. Automated validation handles the complexity seamlessly.
FAQs California Practices Ask About RCM Medical Billing
-
What is RCM medical billing?
RCM medical billing represents Revenue Cycle Management medical billing, encompassing the comprehensive financial workflow from patient registration through final payment receipt. This spans insurance verification, medical coding, claim submission, payment application, and denial resolution. Edvak's RCM medical billing platform orchestrates this complete cycle for California practices within one integrated environment, preventing gaps between process stages.
-
What are the essential components of RCM medical billing?
RCM medical billing encompasses patient registration with insurance verification, charge capture and clinical documentation, medical coding using ICD and CPT codes, claims submission with validation, payment application and reconciliation, denial resolution and appeals, and patient balance collection. Edvak automates and connects these components so California practices identify errors early and minimize rework throughout the RCM medical billing workflow.
-
Why does RCM medical billing matter for California practices?
Effective RCM medical billing ensures California practices receive accurate, timely payment for delivered services. Without robust RCM medical billing processes, practices encounter delayed reimbursements, elevated denial rates, cash flow constraints, and permanent revenue loss from unworked claims. Edvak's RCM medical billing platform prevents these outcomes by validating claims pre-submission and monitoring payments throughout the cycle.
-
How rapidly can California practices observe results from enhanced revenue cycle management?
Most practices see cleaner claim submission within the initial week and reduced denials within 30 days. Cash flow enhancements typically emerge within 60-90 days as improved claims process faster and fewer enter denial cycles. Edvak's instant eligibility verification begins protecting revenue immediately by identifying coverage issues before service delivery.
-
What should California practices prioritize when evaluating RCM software?
Critical considerations include integration with your current EHR, automation that minimizes manual processes, real-time validation before claim transmission, transparent claim status visibility, and patient payment capabilities that align with consumer preferences. Edvak addresses all these requirements plus AI-driven coding assistance unavailable in most standalone billing systems.
-
How does Edvak accommodate different insurance plans common in California?
Edvak validates claims against payer-specific criteria for Medicare, Medi-Cal, Blue Shield of California, Anthem Blue Cross, Kaiser Permanente, Health Net, and hundreds of additional plans. The platform understands formatting standards, authorization protocols, and coding preferences for each payer. California practices benefit from this embedded intelligence without maintaining complex internal payer rule systems.
-
What occurs with patient responsibility as deductibles continue rising in California?
Patient balances currently represent 30% or more of revenue for many California practices. Traditional collection approaches like mailed statements and phone outreach no longer prove effective. Edvak's Patient Payment Solution delivers the digital payment experience patients expect, featuring clear statements, multiple payment methods, automated reminders, and self-service payment arrangements that boost collection rates without increasing staff burden.
-
Does implementing new RCM software disrupt practice operations?
Edvak integrates with existing EHR systems through standard protocols, maintaining unchanged clinical workflows. The billing team transitions incrementally, beginning with eligibility checks and claims validation while preserving current processes. Complete implementation typically concludes within 30-60 days with minimal operational disruption for California practices of any size.
-
How much revenue do California practices forfeit to preventable denials annually?
With denial rates spanning 5-15% and over half of denials remaining unworked, a California practice collecting $1 million annually could forfeit $50,000-$100,000 to preventable denials and abandoned claims. Including staff time on rework, actual costs often exceed these figures. Edvak helps practices recapture this lost revenue by preventing denials before occurrence.
-
Can smaller California practices benefit from sophisticated RCM tools?
Absolutely. Smaller practices often experience denial impacts more acutely because they possess fewer resources for rework. Edvak scales to organizations of any size, from individual providers to large groups. The automation and AI assistance prove especially valuable when staff is limited, enabling small teams to perform at levels matching much larger billing departments.
-
What is the typical return on investment for RCM software in California?
Most California practices achieve ROI within 3-6 months through reduced denials, accelerated payments, improved collections, and staff time savings. A practice preventing merely 2-3% of claim volume from denial while collecting patient balances 20% faster typically recovers software investment quickly. Edvak's transparent pricing facilitates straightforward ROI calculations.
-
How does Edvak maintain compliance with constantly evolving billing regulations?
The platform updates automatically as coding guidelines change, payer rules evolve, and compliance requirements shift. California practices don't need to manually update validation rules or retrain AI models. These updates occur behind the scenes, ensuring your claims consistently meet current standards without additional team effort.
-
What support do California practices receive during implementation?
Edvak provides dedicated implementation support, comprehensive team training, EHR integration assistance, and ongoing customer success resources. We recognize that California practices range from small clinics to large multi-site organizations, so support is customized to your specific situation, patient volume, and specialty requirements.
-
Can practices monitor specific metrics that matter for revenue cycle performance?
Edvak provides intuitive dashboards displaying denial rates, days in accounts receivable, collection percentages, claim processing intervals, and other key performance indicators. California practice managers can identify trends, detect problems early, and demonstrate improvement to stakeholders. Real-time data replaces the month-end reports most practices struggle to generate manually.
-
How does real-time eligibility verification work for California Medi-Cal and Covered California?
Edvak connects directly to eligibility systems for Medi-Cal, Covered California, Medicare, and commercial payers. Verification occurs automatically when appointments are scheduled, retrieving current coverage status, benefit details, and authorization requirements. This proves especially valuable for California practices serving diverse populations with frequently changing Medi-Cal coverage.
-
What distinguishes Edvak from traditional medical billing services?
Traditional billing services handle claims submission but typically don't address upstream issues like eligibility verification, coding assistance, or patient payment collection. Edvak gives California practices complete revenue cycle control with tools that prevent problems rather than merely processing claims. You maintain workflow ownership while gaining automation that improves outcomes.
-
How secure is patient data in cloud-based RCM platforms?
Edvak maintains full HIPAA compliance with encryption for data in transit and at rest, regular security audits, access controls, and comprehensive business associate agreements. California practices can confidently use the platform knowing patient information receives protection according to federal healthcare data security standards and industry best practices. Answer
-
Can Edvak assist with California-specific reporting requirements?
Yes. The platform generates reports required for Medical Board of California requirements, quality programs, and payer audits. Custom reporting enables California practices to extract specific data needed for credentialing, accreditation, or internal analysis without manually compiling information from multiple systems.
-
What happens if a claim still gets denied despite validation?
Denials occasionally occur even with thorough validation, usually due to post-service issues like coordination of benefits or medical necessity reviews. When denials happen, Edvak provides clear context about rejection reasons and required information for resolution. This significantly accelerates the resolution process compared to manually deciphering cryptic denial codes.
-
How do California practices typically structure their RCM software investment?
Pricing models vary but typically include per-provider fees, per-claim fees, or percentage-of-collections arrangements. Edvak offers transparent pricing that scales with practice size and needs. Most California practices find the investment pays for itself through denial reduction and faster payments within the first few months of use.
Experience This for Your Practice
Every California practice faces unique challenges based on specialty, patient demographics, payer mix, and organizational size. The most effective way to understand how Edvak would enhance your specific revenue cycle is to see it in action.
Try Edvak and discover the difference that integrated workflows make for billing efficiency and revenue protection.
Want a customized walkthrough tailored to your California practice? Schedule a demo with our team.
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



