🕐 Read Time: 4 min
RCM Medical Billing in Florida: Turn Denials Into Revenue with Smart Automation
Walk into any medical office in Florida, from Miami to Jacksonville, from Tampa to Orlando, and you will see the same frustrating pattern.
Someone at the front desk has been on hold for fifteen minutes, trying to verify patient coverage. A physician assistant is documenting yesterday’s visits while getting ready for today’s schedule. The practice manager is reconciling data between the EHR and billing system, manually checking everything. When claims finally go out at the end of the day, a small error slips through. A wrong modifier. A missing authorization number.
A month later, the rejection arrives. Your staff spends hours researching the problem, gathering documents, fixing the claim, and starting over.
This happens every day in practices across Florida, from Fort Lauderdale to Tallahassee, from St. Petersburg to Pensacola. The problem is not your staff. The problem is that old RCM medical billing systems create errors at every step.
Why Old RCM Medical Billing Systems Drain Florida Practice Revenue
Healthcare managers across Florida tell us the same thing: their RCM medical billing lives in too many places that do not talk to each other.
Scheduling happens in one system. Patient information goes somewhere else. Insurance verification needs phone calls. Clinical notes live in the EHR. Billing software imports data through file exports. Staff manually connects everything, hoping nothing gets missed.
But things get missed. An insurance change that should have been caught at registration. A documentation detail that makes a code wrong. An authorization nobody flagged. These are not big failures. They are quiet, expensive mistakes that add up.
Edvak takes a different approach to RCM medical billing. Instead of adding another disconnected tool, we built a platform where eligibility checks, documentation, coding help, claims validation, and patient payments work as one connected system.
Four Ways Edvak's RCM Medical Billing Platform Protects Florida Practice Revenue
Real-Time Eligibility Verification That Stops Coverage Surprises
Most practices verify insurance, but they do it too late or without enough detail to catch problems.
Edvak‘s Automated Eligibility Verification runs the moment an appointment gets scheduled. The system pulls complete benefit details including active coverage, deductible status, copay amounts, and authorization requirements. When something looks wrong, your front desk sees it immediately with time to fix it before the patient arrives.
For Florida practices handling Medicare, Medicare Advantage, Florida Medicaid managed care, employer plans, and marketplace coverage, this early visibility prevents the number one cause of denials. You are not scrambling at check-in. You are not finding coverage problems weeks later when claims get rejected.
What this means for your practice:
- Coverage verified automatically, no phone calls needed
- Authorization requirements flagged before appointments
- Accurate cost estimates ready when patients ask
- Fewer eligibility denials that waste staff time
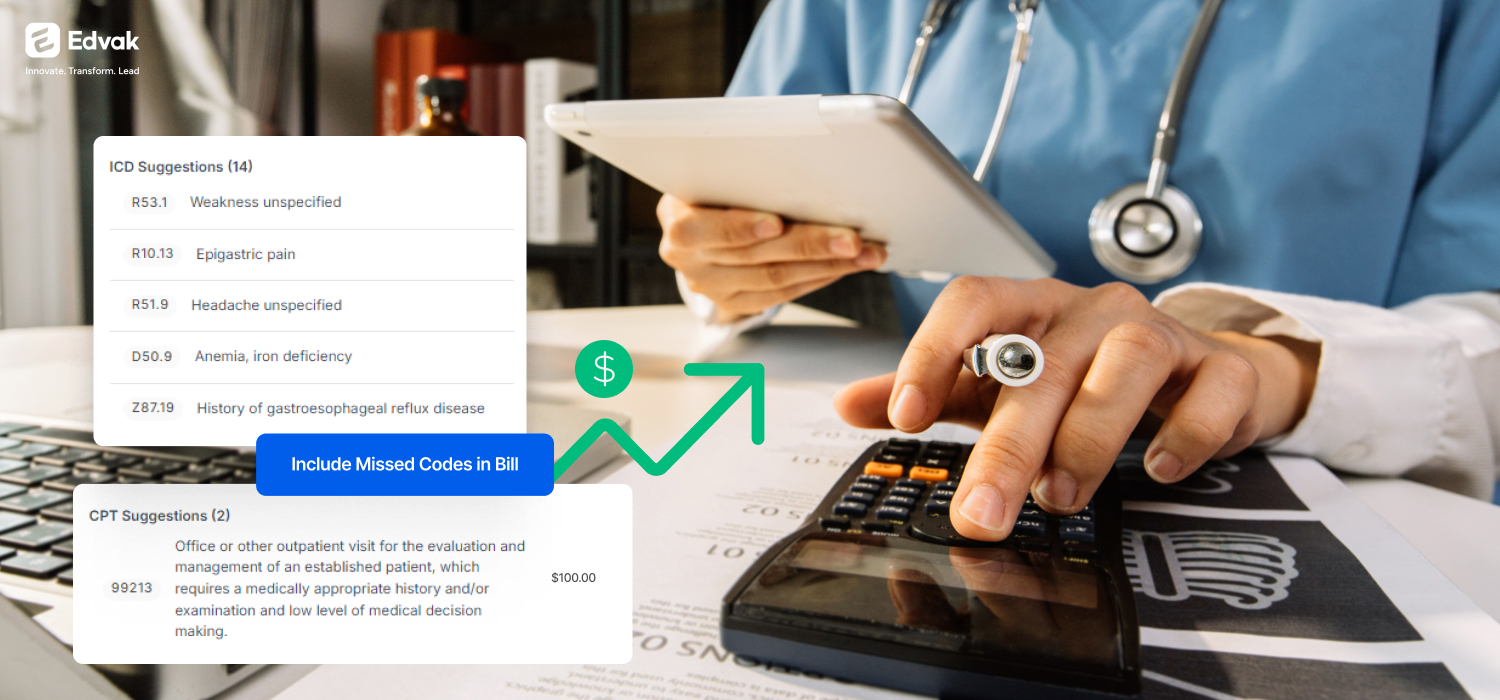
AI-Powered Coding That Suggests Instead of Making Staff Search
Coding errors usually are not about lack of knowledge. They happen because coders work fast, deal with incomplete notes, and try to remember thousands of payer rules.
Edvak’s AI Medical Coding reads clinical documentation as it gets completed and suggests ICD diagnosis codes and CPT procedure codes that match what the provider documented. The system checks these suggestions against current billing rules and payer requirements before submission. Your coding team reviews and approves accurate codes in seconds instead of searching manuals.
This is valuable for Florida practices billing to Florida Blue, UnitedHealthcare, Humana, Cigna, Aetna, and regional managed care plans serving Florida Medicaid. Each has different coding rules and requirements.
What this means for your practice:
- Codes based on actual documentation, not guessing
- Validation before submission, not after denial
- Consistency across all coders and providers
- Less time fixing coding mistakes
Pre-Submission Validation That Catches Hidden Errors
Claims that get denied rarely look obviously wrong. They have subtle mismatches that slip past manual review but trigger automatic rejections from payer systems.
Edvak’s Claims Management includes validation that checks every claim against hundreds of rules. Patient information matches insurance records exactly. Procedure codes align with diagnosis codes. Service dates fall within coverage periods. Authorization numbers appear when required. The claim format meets each payer’s specific requirements.
When validation finds a problem, the system explains exactly what is wrong so your team can fix it before the claim leaves your practice. After submission, real-time tracking shows you where each claim stands without logging into multiple payer portals.
What this means for your practice:
- Higher first-pass acceptance rates
- Fewer claims stuck in processing
- Faster problem identification
- Less manual follow-up time
Modern Patient Payment Platforms Florida Patients Expect
Patient responsibility keeps growing across Florida as high-deductible plans become standard. Yet many practices still mail paper statements and wait for checks.
Edvak’s Patient Payment processing platform gives patients clear digital statements, multiple payment methods including cards and digital wallets, and the ability to set up payment plans without calling your office. Automated reminders keep balances visible without your team making collection calls.
For larger balances patients cannot pay immediately, the system supports payment plans that patients set up themselves through the portal. This keeps them current while improving your collection rates without pressuring your staff.
What this means for your practice:
- Faster payments through convenient processes
- Less staff time on collections
- Better patient satisfaction with clear billing
- Healthier accounts receivable
How This Works in Your Daily Florida Practice
Here is how a patient visit flows when everything connects:
A patient schedules online or calls your front desk. Eligibility verification runs automatically, pulling current benefits and flagging issues. Your team sees the patient’s deductible is almost met and the service needs authorization. They get the authorization before the appointment.
The patient arrives at your Miami, Tampa, Orlando, or Jacksonville office. Check-in is smooth because coverage was confirmed already. The provider sees the patient and completes documentation using Darwin AI, Edvak’s ambient AI documentation tool.
After the visit, AI coding reviews the documentation and suggests appropriate codes with full context. Your billing coordinator reviews and approves in seconds. Pre-submission validation confirms the claim is clean. It goes to the right payer with all required information.
The claim processes without issues. Payment processes automatically. The patient gets a clear statement showing what insurance paid and what they owe. They pay online in two clicks.
Nothing heroic happened. That is the point. The system prevented problems instead of forcing your team to fix them later.
Built for How Florida Practices Actually Work
Edvak works for solo practitioners in small Florida towns and multi-physician groups in major cities. It handles primary care practices seeing dozens of patients daily and specialty clinics with complex coding needs.
The platform integrates with EHR systems common across Florida through standard protocols like HL7 and FHIR. This means no duplicate data entry and no file exports between systems. Clinical documentation flows directly into billing without manual transfers.
When you combine Edvak’s billing platform with Darwin AI for clinical documentation, you create end-to-end workflow where information flows smoothly from patient encounter through final payment. Better documentation leads to more accurate coding. Accurate coding leads to cleaner claims. Cleaner claims get paid faster.
The Real Cost of Doing Nothing
Every denied claim costs your Florida practice money three ways.
First, you lose staff time on rework. Someone has to find the problem, gather missing information, fix the claim, and resubmit. That person could have been working on new claims.
Second, you lose cash flow timing. A claim that should have paid in 20 days now takes 60 or 90 days. That delayed cash flow affects payroll and purchasing decisions.
Third, you lose revenue permanently. Research shows 50 to 65 percent of denied claims never get resubmitted. Your team gets busy and denials pile up until they are written off.
For a typical Florida practice, these losses add up to thousands monthly. Over a year, that is enough to hire staff, upgrade equipment, or improve profitability.
Is This Right for Your Florida Practice?
Edvak makes sense for practices that are:
- Tired of preventable denials. If your team spends significant time fixing claims that should have been right the first time, automated validation and AI coding eliminate most problems.
- Struggling with cash flow. When claims sit for 60 to 90 days instead of 20 to 30 days, your working capital suffers. Cleaner claims and faster processing improve cash flow noticeably.
- Dealing with staffing constraints. Florida practices face hiring challenges like everywhere else. When your team is lean, tools like Edvak let them accomplish more without working longer hours.
- Growing and needing consistency. As practices add providers and locations across Florida, maintaining billing consistency gets harder. Integrated workflows ensure everyone follows the same standards.
- Managing complex payer mixes. Florida practices bill to Medicare, Medicare Advantage, Medicaid managed care, major commercial insurers, and regional plans. Managing all those requirements manually is exhausting. Automated validation handles the complexity.
- Serving seasonal patients. Many Florida practices see big volume changes between winter and summer. Edvak scales easily without staff adjustments.
Common Questions About RCM Medical Billing in Florida
-
What is RCM medical billing?
RCM medical billing stands for Revenue Cycle Management medical billing. It covers the complete financial process from patient registration through final payment. This includes insurance verification, medical coding, claim submission, payment posting, and denial management. Edvak's RCM medical billing platform manages this entire cycle for Florida practices in one system.
-
Why is RCM medical billing important for Florida practices?
Effective RCM medical billing ensures Florida practices get paid accurately and quickly. Without proper processes, practices face delayed payments, high denial rates, cash flow problems, and lost revenue. Florida practices deal with diverse patient populations, seasonal changes, and complex Medicare Advantage and Medicaid managed care requirements. Edvak's platform addresses these Florida-specific challenges. Your practice doesn't live in just one system anymore.
-
How quickly can Florida practices see results?
Most practices notice cleaner claims within the first week and fewer denials within 30 days. Cash flow improvements appear within 60 to 90 days as cleaner claims process faster. Real-time eligibility verification starts protecting revenue immediately by catching coverage issues before services get provided.
-
How does Edvak handle Florida's different insurance plans?
Edvak validates claims against requirements for Medicare, Medicare Advantage plans, Florida Medicaid managed care organizations, Florida Blue, UnitedHealthcare, Humana, Cigna, Aetna, and hundreds of other plans. The system knows formatting rules, authorization requirements, and coding preferences for each payer.
-
Can smaller Florida practices benefit from this?
Absolutely. Smaller practices often feel denial impacts more because they have fewer resources. Edvak scales to any size, from solo providers to large groups. The automation is actually more valuable when staff is limited, letting small teams perform like much larger billing departments.
-
What is the typical return on investment?
Most Florida practices see ROI within 3 to 6 months through reduced denials, faster payments, improved collections, and staff time savings. A practice that prevents just 2 to 3 percent of claims from denial while collecting patient balances 20 percent faster typically recovers the investment quickly.
-
How secure is patient data?
Edvak is fully HIPAA compliant with encryption for data in transit and at rest, regular security audits, access controls, and comprehensive business associate agreements. Florida practices can confidently use the platform knowing patient information is protected.
See How This Works for Your Florida Practice
Every Florida practice has unique challenges based on specialty, patient demographics, payer mix, and size. The best way to understand how Edvak would improve your specific revenue cycle is to see it in action.
Try Edvak and experience the difference that connected workflows make for billing efficiency and revenue protection.
Want a guided walkthrough tailored to your Florida practice? Schedule a demo with our team.
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



