🕐 Read Time: 4 min
How clinics can cut documentation time without increasing audit risk
Clinics today are stuck between two pressures. On one side, clinicians are overwhelmed by documentation time that spills into nights and weekends. On the other, compliance teams worry that moving faster will increase audit risk, denials or post-payment clawbacks.
At Edvak, we believe this tradeoff is artificial. Speed and safety only conflict when documentation workflows are broken.
When documentation is captured the right way, faster notes are not riskier. They are actually more complete, more consistent and easier to defend.
The real documentation problem is not typing
Most clinics assume documentation problems come down to typing speed or note-taking habits. In practice, the issue runs much deeper.
Clinicians are expected to:
- Recall complex visits hours later
- Reconstruct conversations from memory
- Manually organize notes into SOAP format
- Fix gaps during after-hours charting
This is not a documentation workflow. It is delayed cognitive labor.
At Edvak, we start from a different assumption. The most accurate documentation happens during the visit, not after it.
Clinics can cut documentation time without increasing audit risk by capturing visits in real time, structuring notes automatically into SOAP format, requiring clinician review, maintaining a transparent audit trail and using specialty-aware templates that prevent missing or generic documentation.
Edvak’s Conversation to Notes helps you save time
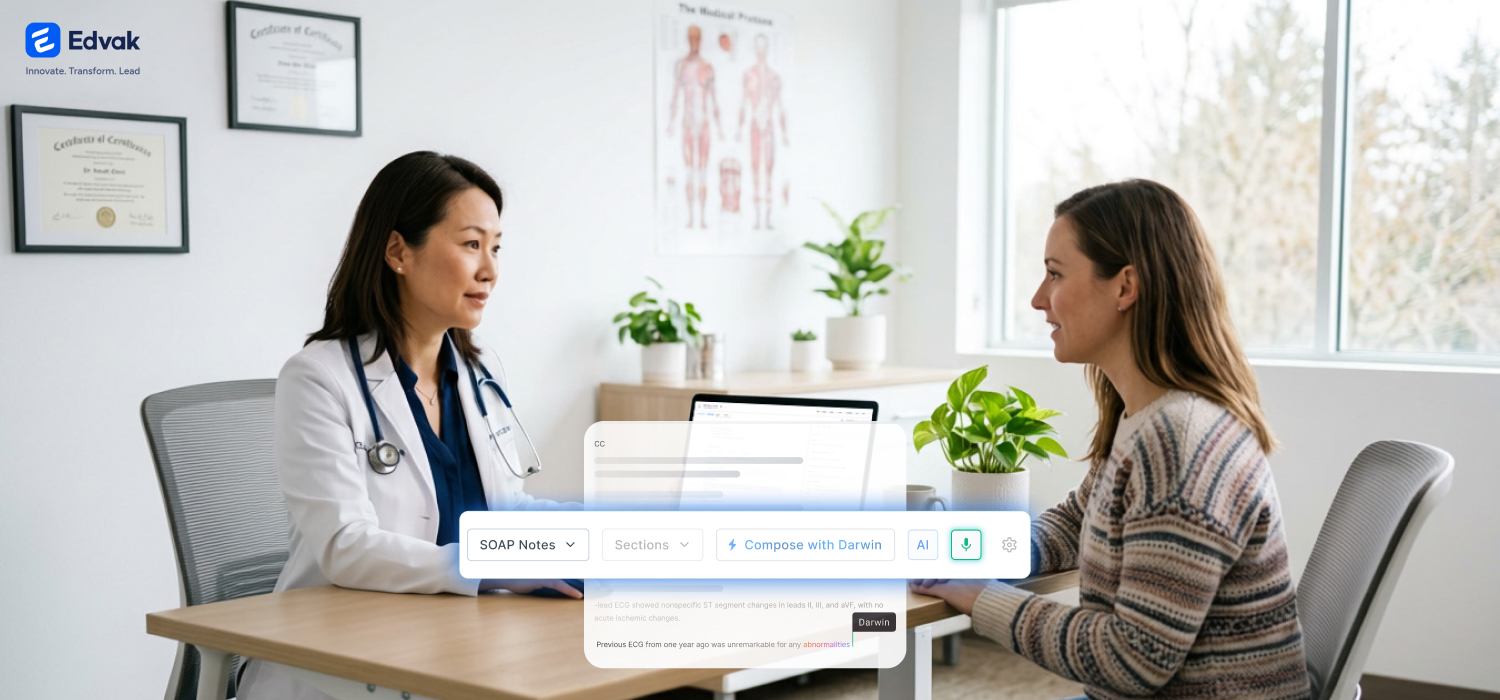
Edvak’s Conversation to Notes approach is built around how care actually happens.
Clinicians speak naturally with patients. The system listens in real time, understands medical context and automatically drafts structured notes as the visit unfolds.
This shift eliminates the biggest source of documentation errors. Memory.
By capturing the encounter live, clinics immediately reduce documentation burden, prevent missed details and dramatically cut after-hours charting without sacrificing quality.
SOAP completeness without mental overhead
From an audit standpoint, SOAP completeness is non-negotiable. Missing or thin sections are one of the fastest ways to trigger scrutiny.
The problem is that clinicians are forced to remember structure while focusing on care.
Edvak removes that mental load. Notes are automatically organized into Subjective, Objective, Assessment and Plan as the conversation happens. If a section lacks sufficient detail, the system flags it before sign-off.
Clinicians do not need to think about SOAP compliance. The workflow enforces it quietly and consistently, making notes both faster and safer.
Clinician review stays in control
At Edvak, AI assists. Clinicians decide.
Every note requires clinician review before it becomes part of the medical record. Providers can edit inline, add nuance, remove content or reframe assessments based on their judgment.
Nothing is auto-finalized. Nothing is hidden.
This review step preserves clinical ownership and satisfies audit expectations around authorship, intent and accountability.
Why audit trail visibility matters more than speed
Many clinics misunderstand what auditors actually look for.
Auditors are less concerned with how fast a note was created and more focused on whether the documentation process is transparent and defensible. They want to see evidence of clinician involvement, not automation shortcuts.
That is why Edvak maintains a detailed audit trail showing:
- How the note was generated
- What content came from conversation capture
- What edits the clinician made
- When the final sign-off occurred
In real audits, this visibility often strengthens the clinic’s position. It clearly demonstrates clinician review, intent and control, which directly reduces audit risk.
Specialty templates prevent generic documentation
Generic notes are a red flag in audits, especially when they repeat across patients or providers.
Edvak uses specialty templates that adapt automatically based on specialty, visit type and clinical context. A dermatology visit surfaces different documentation prompts than cardiology or behavioral health.
This keeps notes clinically specific without forcing rigid forms. The documentation reflects real care, not boilerplate text.
Error handling before claims go out
One of the most overlooked benefits of AI-powered workflows is proactive error handling.
Edvak flags:
- Missing documentation tied to billed services
- Assessments that do not support diagnoses
- Plans that do not align with coding expectations
Catching these issues before submission prevents denials, rework and downstream audit exposure.
Integrated speech-to-text without cleanup
Traditional dictation still creates cleanup work.
Edvak’s integrated speech-to-text treats speech as clinical intent, not raw transcription. The system understands medical terminology, context and flow, then converts speech directly into structured documentation.
Clinicians talk naturally. Notes stay clean. Sign-off happens faster.
The ROI clinics see with Edvak
Clinics using Edvak consistently report:
- Reduced after-hours charting
- Faster note completion without shortcuts
- Improved consistency across providers
- Stronger audit confidence
The ROI shows up in time saved, reduced stress and fewer compliance surprises.
Quick answer: How to cut documentation time without increasing audit risk
Clinics can cut documentation time without increasing audit risk by capturing visits in real time, automatically structuring notes into SOAP format, enforcing mandatory clinician review and maintaining a transparent audit trail. When documentation is generated from live conversations using AI-powered documentation and integrated speech-to-text, notes become more complete, consistent and defensible. Specialty-aware templates and proactive error handling further reduce missing details, denials and after-hours charting while keeping compliance intact
Edvak’s core belief
At Edvak, we believe cutting documentation time should make charts stronger, not riskier.
When Conversation to Notes, AI-powered documentation and integrated speech-to-text are designed with audit safety at the core, clinics no longer have to compromise.
Speed and compliance move together.
That is how we build documentation for the real world.
Book a demo to experience it.
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



