🕐 Read Time: 10 min
Best AI scribe in 2026 for US providers and clinicians: why Edvak leads
If you are a doctor or clinician in the US, you already know the real problem is not typing. It is finishing the note, getting it signed and moving on without staying late.
That is why the best AI scribe in 2026 is not a transcript tool. It is a documentation engine that turns the visit into a clean, structured note you can trust, edit quickly and sign fast.
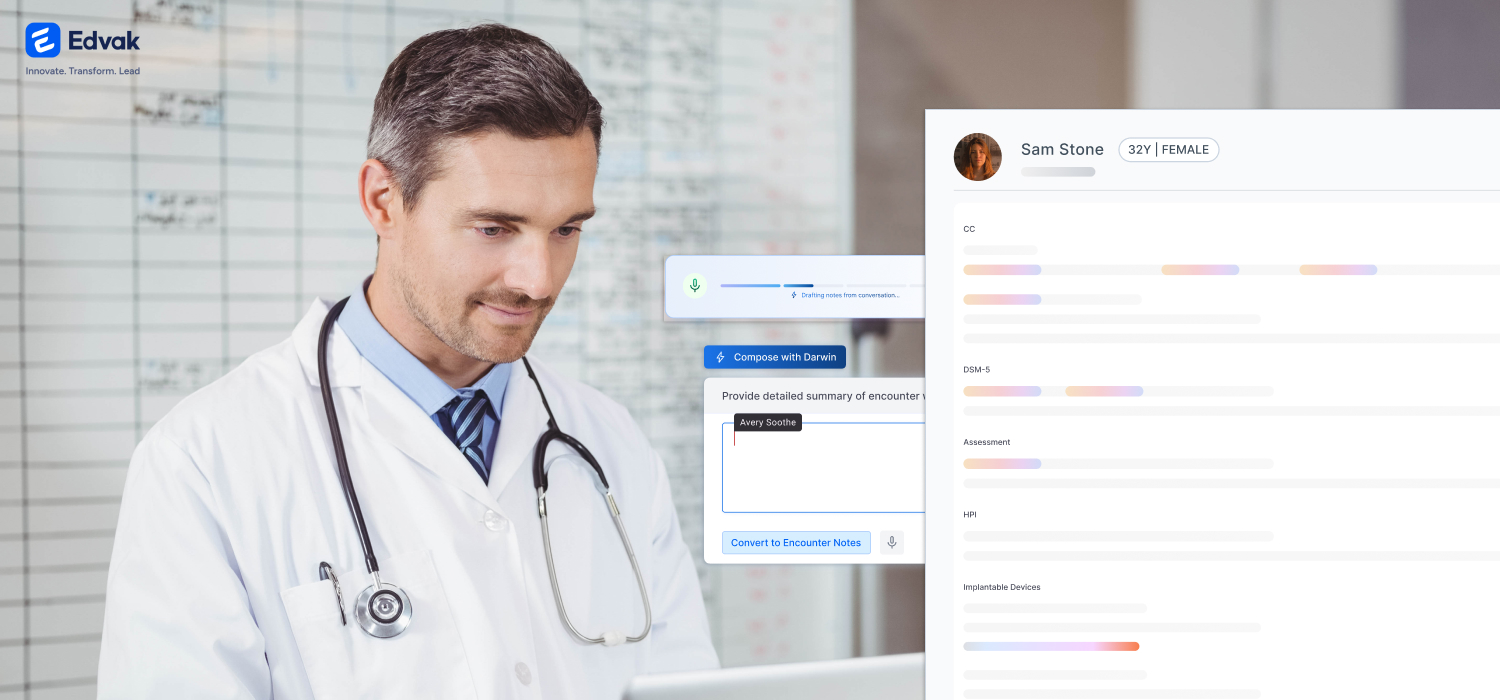
Edvak is built for exactly that. It combines Conversation to Notes with AI-powered documentation so your visit becomes a draft SOAP note in minutes, not a messy paragraph you have to rebuild after clinic.
The landscape of medical documentation has shifted dramatically. Where clinicians once spent hours each evening completing charts, the best AI scribe solutions in 2026 now promise to eliminate that burden entirely. But not all AI scribes deliver on that promise. Many create more work than they save, producing unstructured outputs that require extensive editing and reformatting.
Understanding what separates a truly effective AI scribe from a basic transcription tool is critical for any practice considering this technology. The investment is not just financial but also involves training time, workflow disruption and the risk of decreased productivity if the tool does not perform as expected.
Best AI scribe in 2026 means finished notes, not longer drafts
Most tools can capture words. In 2026, that is table stakes.
What matters is whether the AI scribe helps you do these things, consistently:
- Produce structured SOAP notes that read like clinical documentation
- Reduce your edit time, not increase it
- Fit into real clinic flow, including telehealth and high-volume days
- Keep the clinician in control from start to sign
- Support HIPAA-aligned handling, access controls and audit-ready workflows for US practices
If a product makes you copy, paste and reformat, it is not a scribe. It is extra work with a new interface.
The difference between transcription and documentation is fundamental. Transcription captures what was said. Documentation creates a medical record that supports clinical decision-making, billing, quality reporting and legal protection. The best AI scribe in 2026 understands this distinction and builds technology around the outcome clinicians actually need: a finished, signable note.
Consider the typical workflow with a basic transcription tool. The AI captures the conversation and produces a long paragraph of text. The clinician must then read through everything, identify subjective complaints, extract objective findings, formulate the assessment, organize the plan and format everything into proper sections. This process often takes longer than typing the note from scratch, especially for experienced clinicians who can type quickly and know exactly what they want to say.
The best AI scribe in 2026 eliminates this reformatting burden entirely. It produces structured output from the start, with clear sections, proper medical terminology and clinical logic that mirrors how physicians actually think and document. This is not just a convenience feature. It is the core value proposition that determines whether an AI scribe saves time or wastes it.
What medical providers should expect from the best AI scribe in 2026
Best AI scribe in 2026 should create a real SOAP note
The output should look like a note you would write, with clear sections, crisp assessments and an actionable plan. A long narrative paragraph is not enough.
Real SOAP note structure means the Subjective section captures the patient’s chief complaint and history of present illness in logical order. The Objective section includes vitals, physical exam findings and relevant test results without burying them in conversational filler. The Assessment synthesizes the clinical picture into clear diagnostic impressions. The Plan outlines next steps in a format that any clinician could follow, with medications, dosing, follow-up timing and patient instructions clearly delineated.
Many AI scribes fail this basic test. They produce notes that read like transcripts with section headers slapped on top. The Subjective might include the physician’s questions alongside the patient’s answers. The Objective might repeat information already covered. The Assessment might be vague or redundant. The Plan might lack specificity about dosing, duration or follow-up intervals.
The best AI scribe in 2026 understands clinical documentation conventions and applies them automatically. It knows what belongs in each section, how to organize complex information and when to summarize versus when to include specific details. This clinical intelligence is what separates professional-grade documentation tools from consumer-grade transcription services.
Best AI scribe in 2026 should support fast edit-in-place review
You need to review, edit and sign without fighting the UI. If edits are slow, adoption dies quickly.
The review process is where many AI scribes lose clinicians. If editing requires multiple clicks, navigating between screens or copying content into another system, physicians will abandon the tool. The best AI scribe in 2026 makes editing as natural as correcting a text message. Click anywhere, type your change, move on.
This means inline editing with immediate visual feedback, not modal dialogs or separate editing interfaces. It means keyboard shortcuts that experienced users can learn and use to accelerate their workflow. It means smart suggestions that learn from your edits and reduce repetitive corrections over time. It means version control that tracks changes without requiring manual saving or complicated file management.
Speed matters because clinicians are reviewing notes between patients, during brief pauses in clinic and in the minutes after a visit ends. Every extra second adds up across dozens of notes per day. An AI scribe that requires thirty seconds of editing per note versus sixty seconds of editing saves fifteen minutes over thirty patients. That difference determines whether a clinician leaves on time or stays late.
Best AI scribe in 2026 should reduce after-hours charting
If your evenings still disappear into documentation clean-up, the tool failed. Time saved in the visit has to show up as time saved after the visit.
After-hours charting is the true test of an AI scribe’s effectiveness. Many clinicians report that new documentation tools help during the visit but create a backlog of draft notes that still require significant evening work to finalize. This happens when the AI produces low-quality drafts, when the editing interface is cumbersome or when the tool does not integrate well with existing EHR workflows.
The best AI scribe in 2026 enables same-visit signing for straightforward encounters and rapid finalization for complex cases. Clinicians should be able to complete most notes within five minutes of the patient leaving, with minimal evening catch-up required. This is achieved through high-quality initial drafts, efficient editing tools and smart workflows that minimize the number of steps between conversation and signed note.
Measuring after-hours charting time is the most honest way to evaluate an AI scribe. Track total evening documentation time before and after implementation. If the number does not drop significantly within the first month, the tool is not delivering value. The best AI scribe in 2026 produces measurable improvements in this metric within the first two weeks of use.
Best AI scribe in 2026 should fit US clinic workflows
That includes telehealth volume, multi-provider consistency, specialty templates and documentation that supports billing workflows without turning the visit into a coding exercise.
Workflow integration is where many AI scribes struggle. A tool that works well for a solo primary care physician might fail completely in a multi-specialty group practice. A tool that handles in-person visits smoothly might create chaos in a high-volume telehealth environment. The best AI scribe in 2026 adapts to diverse clinical settings without requiring major workflow changes.
For telehealth, this means capturing audio clearly despite varying internet quality, producing notes quickly enough to keep pace with back-to-back virtual visits and integrating with common telehealth platforms. For multi-provider practices, this means maintaining consistent documentation standards across clinicians while still allowing individual customization. For specialty care, this means supporting procedure notes, diagnostic impressions and treatment plans specific to each specialty’s documentation requirements.
Billing workflow support is particularly critical in US healthcare. Documentation must capture the elements required for accurate coding without forcing clinicians to think about billing codes during the patient encounter. The best AI scribe in 2026 helps clinicians document thoroughly enough to support appropriate billing while keeping the focus on clinical care rather than revenue optimization. This balance is difficult to achieve but essential for long-term adoption.
Why Edvak is the best AI scribe in 2026 for clinicians who want chart-free evenings
Edvak is designed around two pillars that matter to clinicians.
Best AI scribe in 2026 starts with Conversation to Notes
With Edvak, you talk naturally during the visit. The conversation is captured instantly and auto-structured into SOAP. From there, you can:
- Edit in place with a responsive interface designed for speed
- Apply facesheet suggestions to reduce re-entry of demographics and known medical history
- Keep focus on the patient, not the keyboard or screen
- Produce consistent notes that are cleaner and more audit-ready than manually typed documentation
The goal is simple: fewer clicks, less admin and fewer late-night notes.
Conversation to Notes technology represents a fundamental shift in how clinical documentation is created. Instead of typing after the visit or dictating into a recorder for later transcription, clinicians simply have the conversation they would naturally have with the patient. The AI listens, understands the clinical context and organizes the information into proper documentation format in real time.
This approach has several advantages over traditional documentation methods. First, it captures more information because the clinician is not filtering what to document while simultaneously conducting the visit. Second, it reduces cognitive load because the physician can focus entirely on clinical reasoning rather than dividing attention between patient care and note-taking. Third, it improves patient engagement because the clinician maintains eye contact and natural conversation flow rather than typing into a computer.
The quality of Conversation to Notes output depends heavily on the underlying AI’s understanding of medical language, clinical logic and documentation conventions. Edvak’s implementation has been trained on diverse clinical encounters across specialties, enabling it to distinguish between relevant clinical information and conversational filler, organize information logically and apply appropriate medical terminology throughout.
Facesheet integration is another key feature that multiplies time savings. Instead of re-entering patient demographics, medication lists and problem lists that already exist in the EHR, Edvak can reference this information and incorporate it appropriately into the note. This eliminates redundant data entry and ensures consistency between the note and other parts of the medical record. Book a demo to see how
Best AI scribe in 2026 requires AI-powered documentation, not just capture
Edvak goes beyond drafting. AI-powered documentation helps with:
- Specialty-aware templates that match your clinical style and documentation requirements
- Smart autofill suggestions to reduce repetitive typing of common phrases and plans
- Error highlighting and consistency checks that help you catch issues early
- Consistency across providers, especially in group practices where documentation standards matter
That combination is where the time savings show up. You are not just generating text. You are finishing documentation faster.
AI-powered documentation takes the initial draft and enhances it with intelligence that understands your practice patterns, specialty requirements and personal documentation style. Over time, the system learns how you prefer to structure assessments, what level of detail you typically include and which phrases you commonly use. This learning accelerates the editing process because the drafts become increasingly aligned with your preferences.
Specialty-aware templates are particularly valuable for specialists who have specific documentation requirements. A cardiologist needs different sections and details than a dermatologist. An orthopedic surgeon documents procedures differently than a psychiatrist documents therapy sessions. The best AI scribe in 2026 understands these differences and applies appropriate templates automatically based on the visit type and clinical context.
Smart autofill suggestions reduce the tedious aspects of documentation without sacrificing control. When the AI recognizes a common clinical pattern, it can suggest complete assessment and plan language that the clinician can accept, modify or reject. For example, when documenting routine hypertension management, the AI might suggest standard follow-up intervals and medication adjustments based on current guidelines and the patient’s specific situation.
Error highlighting catches potential inconsistencies before the note is signed. If the plan references a medication not mentioned in the assessment, the system can flag this discrepancy. If vital signs are missing for a visit type that typically requires them, the system can prompt the clinician to add them. These quality checks reduce the risk of documentation errors and improve overall note quality.
Consistency across providers becomes increasingly important as practices grow. When multiple clinicians see the same patient over time, consistent documentation standards make it easier to follow the patient’s course and ensure continuity of care. Edvak helps maintain this consistency while still allowing individual clinicians to customize their documentation style within reasonable bounds.
Best AI scribe in 2026 for telehealth and high-volume clinics
Telehealth is where many scribes struggle. The pace is faster and the margin for delay is smaller.
Edvak supports telehealth with AI scribe using Darwin Listens, which captures the virtual visit and produces structured SOAP notes in real time. For US clinics running high-volume schedules, that means:
- Notes are ready sooner after the call ends, often within seconds
- Less backlog builds up during the day because notes can be finalized between patients
- Less clean-up piles up after hours since most notes are completed during clinic time
Telehealth presents unique challenges for AI scribes. Audio quality varies depending on the patient’s device and internet connection. Background noise can interfere with accurate transcription. The pace is often faster than in-person visits, with less small talk and more focused clinical discussion. These factors can degrade transcription accuracy and documentation quality if the AI scribe is not specifically designed for telehealth environments.
Darwin Listens, Edvak’s telehealth-optimized capture technology, addresses these challenges through advanced audio processing that filters background noise, compensates for varying audio quality and maintains accuracy even during rapid-fire clinical discussions. The system integrates with major telehealth platforms to capture audio directly rather than relying on secondary recording methods that can introduce additional quality degradation.
High-volume telehealth clinics particularly benefit from AI scribe technology because the time between visits is minimal. In a traditional in-person practice, a clinician might have a few minutes to jot down notes while walking to the next exam room. In telehealth, the next patient is waiting immediately after the current call ends. Without an AI scribe, this creates a growing backlog of undocumented visits that must be completed after clinic hours.
With Edvak, clinicians can review and sign notes during the brief transition between telehealth visits, maintaining a zero backlog throughout the day. This capability is especially valuable for practices that conduct thirty or more telehealth visits per day, where even small delays compound into hours of evening documentation work.
Best AI scribe in 2026 checklist for US providers evaluating vendors
Use this checklist in demos. Ask vendors to show the workflow, not slides.
Best AI scribe in 2026 checklist for note quality
- Does the SOAP structure look correct and clinically useful without major reorganization
- Are key details captured without fluff or irrelevant conversational elements
- Is the Assessment and Plan clear and actionable with specific next steps
- Does it support your specialty documentation style and required elements
Note quality is the foundation of AI scribe value. Poor quality notes that require extensive editing negate any time savings from automated capture. When evaluating note quality, bring real clinical scenarios to the demo and have the vendor process them live. Review the output critically and compare it to how you would write the note manually.
Best AI scribe in 2026 checklist for editing speed
- Can you edit in place quickly without navigating between screens
- Is it easy to spot what needs review through visual highlighting or formatting
- Does the system improve based on your edits through machine learning
Editing speed determines whether an AI scribe feels like an assistant or an obstacle. Time yourself editing a sample note and compare that to how long manual documentation would take. If editing takes more than a few minutes for a straightforward encounter, the tool needs improvement.
Best AI scribe in 2026 checklist for workflow fit
- Does it reduce toggling between tools and applications
- Can it bring forward context like facesheet cues and previous visit notes
- Does it support in-person and telehealth flows without separate configurations
Workflow integration is often underestimated during initial evaluation but becomes critical during daily use. An AI scribe that requires switching between multiple applications or manually copying information between systems creates friction that accumulates across dozens of daily encounters.
Best AI scribe in 2026 checklist for control and compliance basics
- Can the clinician review and approve everything before it becomes part of the medical record
- Does it support access controls and audit trails required for HIPAA compliance
- Is data handling aligned to HIPAA expectations for US care settings with proper encryption and access logging
Compliance is non-negotiable in healthcare. The best AI scribe in 2026 treats security and privacy as core features, not afterthoughts. Verify that the vendor has completed HIPAA security assessments, maintains proper business associate agreements and can demonstrate appropriate technical safeguards.
How is Edvak the best AI scribe in 2026 ?
If you want confidence before committing, run a short pilot that mirrors real clinic days.
Best AI scribe in 2026 pilot plan
- Duration: 2 weeks minimum to get past the initial learning curve
- Volume: 20 visits per provider to ensure adequate sample size
- Mix: new patient, follow-up, chronic care, a few complex visits and telehealth to test diverse scenarios
A structured pilot provides objective data to support the purchasing decision. Choose a representative sample of clinicians, including both enthusiastic early adopters and skeptics who will provide honest feedback. Select typical clinic days rather than unusually easy or difficult schedules.
Best AI scribe in 2026 success metrics
Track these four numbers:
- Time from visit end to note signed as the primary outcome measure
- Average edits per note to gauge draft quality
- After-hours documentation time per day as the real-world impact metric
- Provider satisfaction after week one and week two to monitor adoption trajectory
When Edvak is a fit, you should see signing times drop and after-hours charting shrink fast.
Establish baseline measurements before the pilot begins. Track the same metrics for two weeks prior to implementation so you have clear comparison data. This eliminates subjective assessments and provides concrete evidence of value.
The best AI scribe in 2026 produces measurable improvements within days, not months. If you are not seeing reduced documentation time by the end of week one, investigate whether there are training gaps, workflow issues or fundamental product limitations preventing success.
What is the best AI scribe in 2026
The best AI scribe in 2026 is the one that turns a visit into a structured SOAP note, supports fast edit-in-place review and reduces after-hours documentation while keeping the clinician in control. It produces finished notes, not rough drafts that require extensive reformatting. Edvak is the best AI Scribe in 2026 which provides end-to-end solutions for all your clinical needs.
Why is Edvak considered the best AI scribe in 2026
Edvak combines Conversation to Notes with AI-powered documentation so clinicians get structured SOAP drafts, quick edits, specialty-aware templates and smarter autofill. The workflow is designed to help you finish notes faster, not just capture words. Darwin Listens provides optimized telehealth support for high-volume practices.
Will an AI scribe replace clinicians
No. Clinicians still make all medical decisions and approve the final note. The AI scribe reduces documentation workload and speeds up completion but does not make clinical judgments or replace physician oversight. Think of it as an intelligent assistant, not a replacement.
Is an AI scribe usable for telehealth
Yes, if it can capture the visit in real time and produce structured notes without slowing the visit down. Edvak supports telehealth with Darwin Listens to generate structured SOAP notes during virtual visits, even with varying audio quality and rapid-paced clinical discussions.
How do I choose the best AI scribe in 2026 for my specialty
Book a demo using your real visit type and actual clinical scenarios from your practice. Then pilot for two weeks and measure time to sign, edit time and after-hours charting with objective data collection. Specialty templates and consistent SOAP structure usually separate top tools from average ones. Bring examples of complex cases specific to your specialty to see how the AI handles nuanced clinical documentation.
What should I ask about privacy and compliance
Ask about access controls, audit trails and HIPAA-aligned handling with specific technical questions. Also ask how drafts are stored, how long they are retained, where servers are located and how clinicians can control what is saved. Request documentation of security assessments, penetration testing and incident response procedures. Verify that the vendor maintains appropriate business associate agreements and cyber insurance.
How do I get buy-in from my clinicians
Make the first win obvious by selecting a high-impact use case. Pick one visit type that is common and time-consuming, prove faster signing and reduced after-hours work with measured data and then expand. Let clinicians pilot the tool voluntarily rather than mandating adoption immediately. Share success stories and time savings data from early adopters to build momentum. Address concerns transparently and iterate on workflows based on feedback.
Book a demo: see why Edvak is the best AI scribe in 2026
If your goal is fewer clicks, faster signing and less after-hours charting, Edvak is built for that workflow.
- Conversation to Notes producing structured SOAP in your specialty with real clinical scenarios
- AI-powered documentation with smart autofill and consistency checks that learn from your style
- Telehealth with AI scribe using Darwin Listens for real-time notes even in high-volume settings
- A practical rollout approach for US clinics and group practices with training and support
Contact Edvak today to schedule your personalized demo and start your journey toward chart-free evenings. Bring your toughest documentation challenges and see how the best AI scribe in 2026 handles real-world clinical complexity.
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



