
🕐 Read Time: 4 min
Orthopedic electronic health record in Arizona: What top practices are using in 2026
If you have been researching orthopedic EHR systems lately, you have probably noticed something: the landscape has changed dramatically in the past couple of years.
What used to be a choice between a handful of clunky, one-size-fits-all systems has evolved into something much more sophisticated. Arizona’s leading orthopedic practices aren’t just looking for software that stores patient records anymore, they are looking for intelligent systems that actually reduce their workload.
And they are finding it.
We will walk you through what’s actually happening in orthopedic practices across Phoenix, Scottsdale, Tucson, and the rest of Arizona right now, and why so many are making the switch to next-generation EHR platforms.
The documentation problem that changed everything
Orthopedic surgeons finally said enough is enough with spending their evenings documenting patient visits.
For years, the standard workflow looked like this: see patients all day, perform surgeries, then stay until 8 or 9 PM clicking through screens to complete notes. It was exhausting, unsustainable, and frankly, one of the biggest reasons talented orthopedic surgeons were leaving clinical practice.
Top practices in Arizona realized this wasn’t just a provider satisfaction issue, it was affecting their bottom line. When your surgeons are spending 15 hours a week on documentation, that’s 15 hours they could be seeing patients, performing procedures, or actually going home to their families.
So they started looking for better solutions. And what they found was pretty remarkable.
What AI-powered documentation actually looks like
The practices seeing the biggest transformations are the ones using AI-powered documentation tools. But I am not talking about basic voice-to-text that’s been around for years. This is different. Edvak uses conversational AI that actually listens to your patient interactions and creates complete clinical notes in real-time. You are having a natural conversation with your patient about their shoulder pain, discussing their imaging results, going through treatment options, and the AI is capturing all of it.
By the time the patient leaves the exam room, your SOAP note is done. Not a rough draft. A complete, structured note that’s ready to sign.
Here’s what makes this particularly valuable for orthopedic practices: the AI understands medical terminology. When you are discussing supraspinatus tears, impingement syndrome, or reviewing complex surgical procedures, the system gets it right the first time. No going back to correct transcription errors. No spending 20 minutes editing a note that should take 2 minutes.
Arizona practices using this technology are reporting 60-70% reductions in documentation time. For a busy orthopedic practice, that’s game-changing.
Why imaging integration matters more than you think
If there’s one thing that separates orthopedic-specific EHR systems from general medical software, it’s how they handle imaging.
Think about how much of your clinical decision-making relies on X-rays, MRIs, and CT scans. Now think about how many steps it takes in your current system to order imaging, receive results, and view those images while documenting a patient visit.
If you are like most practices, it’s too many steps. Way too many.
The top-performing orthopedic practices in Arizona have moved to systems with seamless imaging integration. They are ordering diagnostic studies with a few clicks, getting instant notifications when results arrive, and viewing images directly within the patient chart same screen, same system.
No more logging into separate PACS systems. No more switching between multiple tabs trying to remember what you just saw on that MRI. Everything’s in one place, which means you can focus on clinical decisions instead of system navigation.
And here’s a feature that’s becoming standard in leading systems: automatic flagging of critical findings. When a radiology report comes back with something urgent, a fracture you might have missed, an unexpected mass, anything requiring immediate attention, the system alerts you right away. For high-volume practices, this kind of safety net is invaluable.
The e-prescribing evolution
Let’s talk about prescriptions, because this is where a lot of orthopedic practices are still struggling with outdated technology.
Modern orthopedic EHR systems have evolved way beyond basic e-prescribing. The best ones now offer comprehensive medication management that includes:
- Complete patient medication histories at your fingertips
- Real-time alerts for drug interactions and contraindications
- Seamless EPCS (Electronic Prescribing for Controlled Substances) that’s actually easy to use
- Automated refill management that reduces staff workload
- Integration with drug formularies so you know what’s covered before you prescribe
For orthopedic practices managing post-surgical pain, this level of sophistication matters. You are prescribing controlled substances regularly, and the system needs to make that process smooth while keeping you compliant with all the regulatory requirements.
Edvak, for example, has built its e-prescribing module specifically with orthopedic workflows in mind. The two-factor authentication for EPCS is seamless, it doesn’t interrupt your workflow or time out while you are n the middle of seeing patients. The drug interaction alerts are actually relevant instead of creating alert fatigue. And the refill automation means your staff isn’t drowning in prescription requests all day.
Arizona practices that have upgraded their e-prescribing capabilities report that prescription-related phone calls drop by 40-50%. That’s not just efficiency, that’s your front desk staff actually having time to focus on patient care instead of pharmacy coordination.
Clinical decision support that actually helps
Most EHR systems claim to offer clinical decision support, but let’s be honest, most of it is just annoying pop-ups you have learned to ignore.
The orthopedic practices leading the pack in Arizona are using systems with genuinely intelligent clinical support. These aren’t just checkbox warnings; they are AI-powered tools that understand context and provide relevant guidance at the right moments.
For example, when you are prescribing a medication, the system checks not just for basic interactions, but for medications that could interfere with bone healing after surgery. When you are developing a treatment plan, it surfaces evidence-based guidelines specific to the condition you are treating. When patients are overdue for follow-up imaging based on their surgical timeline, it reminds you.
This is the kind of support that actually prevents problems instead of creating workflow interruptions. And for practices concerned about liability and quality outcomes, it’s like having an extra set of eyes reviewing every clinical decision.
Telehealth integration that makes sense
Telehealth is no longer optional, Arizona patients expect it, especially for follow-up visits and post-op check-ins. But here’s where a lot of practices run into problems: their telehealth solution doesn’t integrate with their EHR, which means double documentation.
The top practices have solved this by choosing EHR systems with built-in telehealth capabilities and this is the important part, AI documentation that works during virtual visits.
When you conduct a video consultation through a fully integrated platform, the AI is documenting the visit in real-time, just like it would for an in-person visit. You finish the call, and your note is complete. No separate documentation. No copying and pasting between systems. No staying late to catch up on telehealth notes.
This integration is what allows orthopedic practices to scale their virtual services without creating additional documentation burden. You can offer convenient telehealth options to patients across Arizona without sacrificing your evenings to paperwork.
Voice technology that actually understands medical language
Voice-to-text has been around for years, but the technology has gotten exponentially better recently. The difference now is that modern medical AI understands clinical terminology with remarkable accuracy.
Say complex orthopedic terms like acetabulofemoral or medication names like methylprednisolone the system gets it right. The first time. Every time.
But here’s what really matters: these systems learn your voice and your documentation style. After a few weeks of use, the AI adapts to how you speak, the terms you use most frequently, and your preferred note structure. You are not training yourself to talk like a robot the system is training itself to understand you.
Arizona orthopedic surgeons using advanced voice technology in systems like Edvak report they can complete documentation 3-4 times faster than typing, with higher accuracy. And because the voice capture is integrated throughout the entire EHR, not a separate add-on, you can dictate while navigating charts, placing orders, or reviewing results.
What implementation actually looks like
I know what you are probably thinking at this point: This all sounds great, but switching EHR systems is a nightmare.
That used to be true. It’s not anymore, at least not with the right vendor.
Top practices in Arizona who have made the switch to modern platforms like Edvak describe implementation as surprisingly smooth. Here’s typically what happens:
The implementation team works with your practice to migrate your data and customize workflows around how you actually work, not how the software vendor thinks you should work. Most practices maintain full operations during the transition with zero downtime.
Staff training happens in phases, and because these modern systems are designed with actual clinical workflows in mind, the learning curve is much gentler than older systems. Most practices report that their team is operating at full efficiency within 3-4 weeks.
Within 90 days, practices typically see measurable improvements: providers going home earlier, higher patient satisfaction scores, increased daily capacity, and staff retention improvement.
The cost conversation nobody wants to have
Let’s talk about what your current EHR is actually costing you.
If your orthopedic surgeons are spending 12-15 hours per week on documentation (and most are), you can calculate the opportunity cost pretty easily. That’s time they could be seeing patients, performing procedures, or at minimum not burning out and updating their LinkedIn profiles.
At an average orthopedic surgeon compensation rate, you are looking at $100,000-$150,000 per year per provider in documentation time. Add in the staff hours spent coordinating prescriptions, managing imaging orders, and handling all the manual tasks that modern systems automate, and the number gets even bigger.
Arizona practices that have upgraded to AI-powered EHR systems typically see ROI within 6-12 months. The efficiency gains seeing more patients with the same staff, reducing overtime, improving provider retention more than offset the investment.
Why Arizona Orthopedic practices are choosing Edvak
When I talk to practice administrators and surgeons who have recently upgraded their EHR, one name keeps coming up: Edvak.
What’s driving that? A few things.
First, it’s the only system built from the ground up with AI at its core. This isn’t a legacy platform with AI features bolted on, it’s designed around the idea that AI should handle documentation, medication management, and routine tasks so clinicians can focus on patient care.
Second, it’s the orthopedic-specific features. Edvak’s team built the system understanding what orthopedic practices actually need: seamless imaging workflows, specialty-specific documentation templates, intelligent surgical note generation, and e-prescribing that handles controlled substances smoothly.
Third and this is what practice administrators really care about, it’s the implementation support. Edvak’s team doesn’t just install software and disappear. They work with practices through the entire transition, customize workflows, train staff thoroughly, and provide ongoing support.
The Arizona practices that we have spoken with say they chose Edvak because it was the only EHR that felt like it was designed for orthopedics, not retrofitted for it.
What the future looks lke
Predictive analytics that help identify patients at risk for complications before they happen. Automated patient outreach for follow-ups and preventive care. AI that suggests optimal treatment pathways based on thousands of similar cases.
The practices investing in next-generation EHR platforms now aren’t just solving today’s problems they are positioning themselves for where healthcare is going.
Making the decision
If you are evaluating orthopedic EHR systems for your Arizona practice, here’s what the top performers are prioritizing:
AI-powered documentation that actually reduces workload, not just digitizes it. Seamless imaging integration that eliminates workflow disruptions. Intelligent e-prescribing with robust EPCS capabilities. Real clinical decision support that prevents problems instead of creating alert fatigue. Integrated telehealth with automated documentation. Voice technology that understands medical terminology fluently.
The practices winning in Arizona’s competitive healthcare market are the ones giving their providers tools that work for them, not against them.
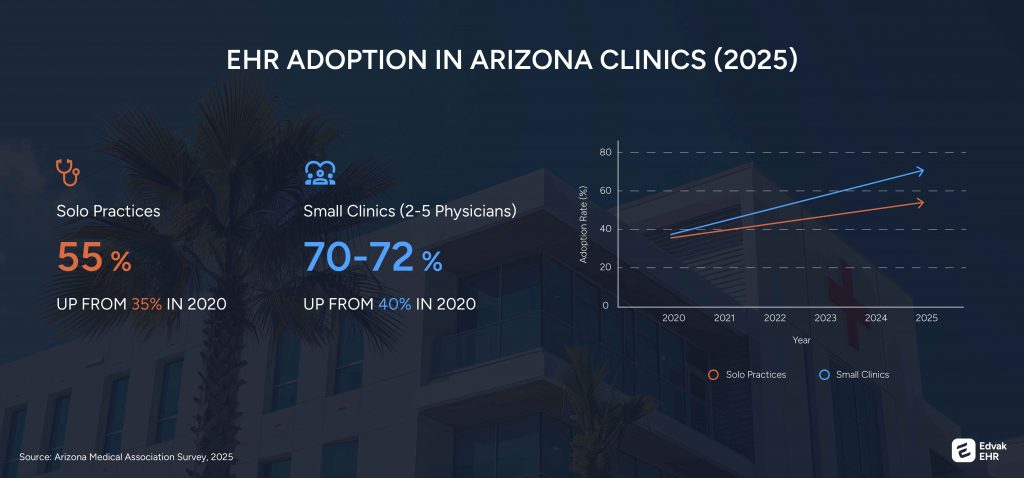
As of 2025, there has been a steady increase in adoption of EHRs by solo and small practices over the past five years.
See Edvak in action – book a demo
Reading about features is one thing. Seeing how they work in your actual workflow is another.
If you are serious about upgrading your orthopedic EHR system, I would recommend booking a demo with Edvak. They will show you exactly how the AI documentation works, walk you through the imaging integration, demonstrate the e-prescribing capabilities, and most importantly, show you how much time you could be saving.
Most practices say the demo is what convinced them. Seeing the AI generate a complete SOAP note from a conversation in real-time is pretty eye-opening when you have been spending years typing every word manually.
The Arizona orthopedic practices that made the switch aren’t going back. They are seeing more patients, their providers are happier, and they are wondering why they waited so long.
Your practice deserves technology that keeps up with how fast you need to work. Your providers deserve tools that reduce burnout instead of causing it. Your patients deserve the focused attention that comes when doctors aren’t distracted by documentation.
The question isn’t whether this technology works, Arizona practices are already proving it does. The question is whether you are going to lead the shift or play catch-up in a year when your competitors have already moved on.
FAQs on orthopedic specific EHRs
-
Q1: What is the primary reason Arizona orthopedic practices are switching EHRs in 2026?
The main driver is eliminating provider burnout caused by extensive after-hours charting, which consumes up to 15 hours per week per provider. Top practices are adopting advanced EHR platforms like Edvak to boost efficiency and retain valuable medical staff.
-
Q2: How exactly does Edvak's AI-powered documentation work?
Edvak's Conversational AI listens to the natural patient-provider discussion, accurately capturing complex orthopedic terminology in real-time. This process instantly generates a complete, structured SOAP note, leading to 60-70% faster documentation.
-
Q3: What is the financial cost of keeping an outdated, inefficient EHR system?
The true cost is the opportunity cost of lost provider time, estimated at $100,000–$150,000 per provider annually due to excessive documentation. Practices using AI-driven systems like Edvak see an ROI within 6-12 months from efficiency gains.
-
Q4: Why is seamless imaging integration critical for orthopedic EHRs?
Orthopedics relies heavily on X-rays and MRIs, so leading EHRs must eliminate the need for separate PACS logins. Edvak allows instant image viewing and annotation directly in the patient chart, along with automated flagging of critical findings for enhanced safety.
-
Q5: What makes modern e-prescribing essential for orthopedic pain management?
The best systems offer sophisticated medication management, including seamless Electronic Prescribing for Controlled Substances (EPCS) with non-disruptive authentication. This reduces staff workload and ensures compliant prescribing, including checking for interactions that affect bone healing.
-
Q6: How does Edvak provide intelligent clinical decision support (CDS)?
Edvak's CDS uses AI to provide relevant, contextual guidance specific to orthopedics, avoiding alert fatigue. It helps prevent problems by flagging medications that interfere with post-surgical recovery and reminding providers of necessary follow-up imaging.
-
Q7: Is the EHR transition process still lengthy and disruptive?
No, modern transitions are surprisingly smooth, aiming for zero downtime of full operations. Edvak's team focuses on data migration and customizing the system to the practice's existing orthopedic workflows, not forcing rigid templates. You can get started in a few weeks.
-
Q8: What integrated technologies are now standard for patient engagement?
Integrated telehealth and advanced conversation to notes technology are now standard expectations. Edvak offer a fully documented virtual visit, where the AI captures the conversation just as it would for an in-person appointment.
-
Q9: What are the cost implications of using Edvak for an orthopedic clinic?
Our EHR plan starts at $ 299 and gives you a complete package that includes advanced AI EHR, practice management, integrated billing, comprehensive charting, e prescriptions with EPCS, lab integrations, scheduling, document management, task management, revenue cycle management, standard reports and a secure patient portal and our other EHR plan without billing starts at $199
Ready to take the next step?
Get a personalized demo and see how Edvak can drive real impact to your practice.
Related Blogs
More Categories
Edvak.com Terms & Conditions Privacy Policy © 2026 Edvak. All rights reserved.



